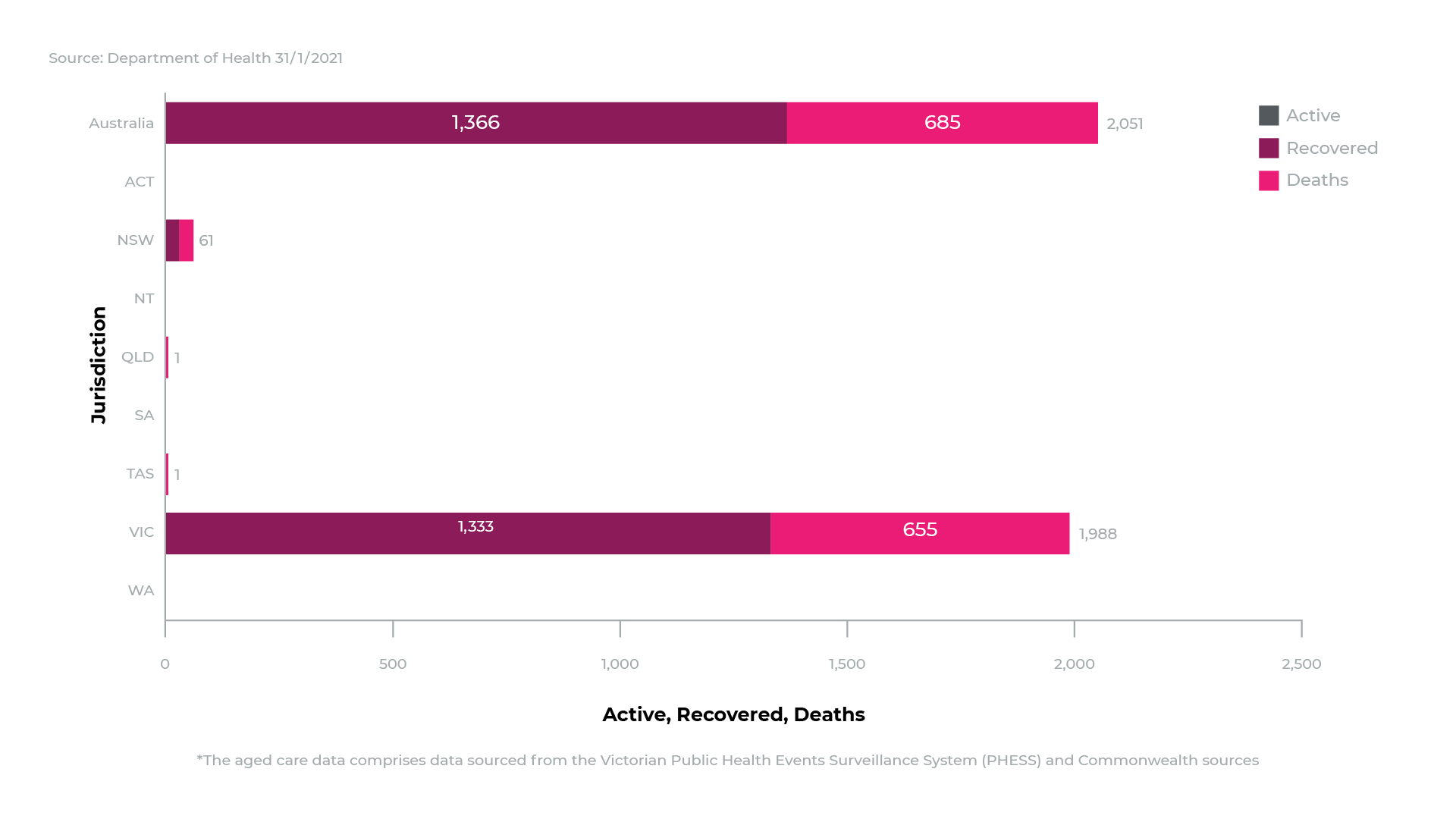
*accurate at 31.01.2021
It’s a deeply saddening number of preventable deaths.
And although COVID-19 has brought hygiene to the front of our minds, this was a problem long before March 2020.
Over the years 2012-2014, 4308 people in aged care died from influenza and pneumonia, and 2350 died from septicemia.
These are not marginal numbers.
These are mothers and fathers, grandmothers and grandfathers dying too soon because their bodies couldn’t fight an accidentally transferred infection.
Simple infection control precautions will stop these deaths and protect your vulnerable residents.
Start with the Right Mindset
Before rushing to a PPE stockpile solution, stop.
Consider: how do you and your staff treat infection control?
Is hygiene a critical piece of your workflows?
Or is it the afterthought, a quick scrub of the mop when there’s a urine spill, a cloth tossed into a laundry sink?
You may need to reset your facility’s priorities.
It helps to think about infection control from a Work, Health and Safety perspective.
WHS & Infection Control
Australian businesses are accustomed to thinking of WHS as important.
Governments have placed an intense focus on safety since 2011, when Safe Work Australia developed the model WHS laws.
The courts saw 114,435 serious Australian workers’ compensation claims in the 2018-19 year.
Running a facility that’s unsafe for employees and others is costly to your finances and your reputation.
COVID-19 has shown us that infection control also demands this level of respect.
We looked at what the aged care industry could learn from WHS principles in tackling infection control.
Some definitions to start:
A hazard is defined as something that has the potential to cause harm to a person’s health and safety.
Risk refers to the probability and consequences of the hazard materializing.
The Hierarchy of Control
WHS ranks risk management methods in a system called the Hierarchy of Control, as shown below.
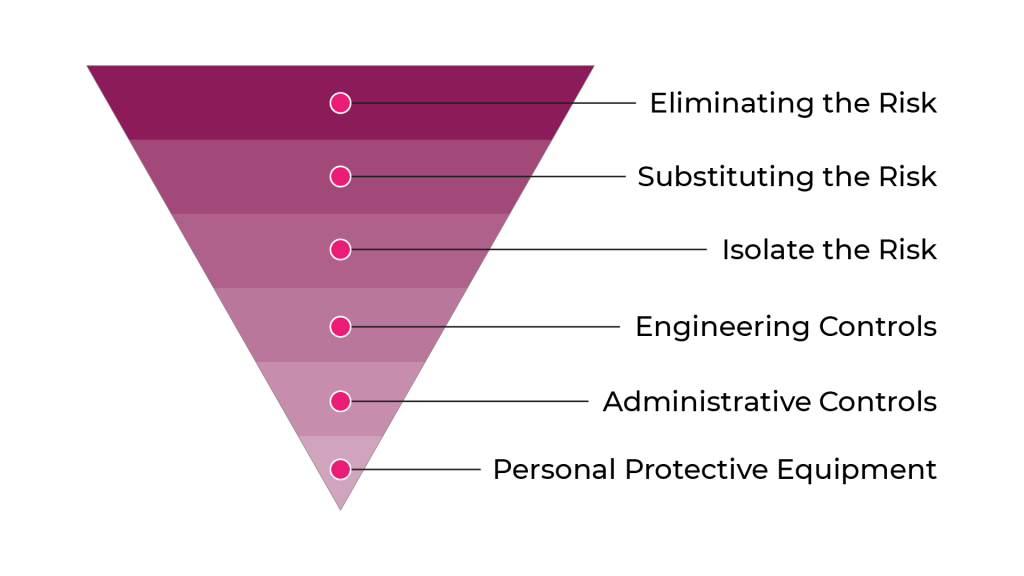
The further down a method is placed, the less effective it is expected to be.
For example, eliminating caustic chemicals from a workspace is much more effective than wearing protective gloves when handling them.
Our Hierarchy of Control, designed specifically for aged care, has 5 steps:
- Eliminate – removing the hazard altogether, so there is “zero chance of a future incident occurring”.
- Substitute – using something safer instead of the hazard.
- Engineer – using physical means to reduce risk.
- Administrate – using rules, procedures, and executive directions to reduce risk, and finally,
- Protect – using personal protective equipment in the risky environment to lower chances of harm.
Hazard: External Visitors
Let’s use the example of “external visitors during a pandemic” to build a Hierarchy of Control.
- Eliminate
Closing aged care facilities to all visitors was common in 2020.
This method is extremely effective, reducing the chance of visitor-borne infections to 0%, but it has drawbacks.
One is the psychological toll taken on aged care residents, when their social circle is abruptly cut off. The Eliminate method increases the risk of harm to mental health and greatly decreases customer experience.
- Substitute
Early in the first Australian lockdowns, innovative aged care staff figured out that ‘no visits’ didn’t have to mean ‘no communication’.
Nurses enabled contact between residents and their loved ones, by substituting physical visits with messaging and video calls.
This method sparked a growth in ‘virtual visits’ which seems likely to continue and has even got Augmented Reality specialists thinking.
- Engineer
The Australian Royal Commission took reports on ‘window visits’ during a COVID-19 outbreak. One report, by aged care industry leaders, stated
Where in-room or in-person visits cannot occur, and the visit is meaningful for residents (e.g. people living with dementia or sensory loss), a window visit may need to be offered.
Royal Commission
into Aged Care Quality and Safety 2020. INDUSTRY CODE FOR VISITING RESIDENTIAL AGED CARE HOMES DURING COVID-19
- Administrate
Facilities also implemented administrative controls for in-person visits.
Some visits were held outside with compliance to social distancing (the visitor stayed 6 or more feet from the resident throughout the visit).
To enforce social distancing, staff often had to attend the visits, causing a significant time cost. While this option increased the ‘reality’ of the experience, it brought a host of risks, including the chance of the virus being transmitted via surfaces and through the air.
- Protect
In-room visits in the resident’s room could be allowed with full PPE worn by the visitor.
The cost of these visits mounted rapidly due to the prices of disposable items such as masks, gowns and gloves.
This option allows for more private visits, however it still has drawbacks, with the PPE making it difficult for the resident to recognize the visitor. Sometimes, the resident would become confused, endangering themselves by trying to take off the visitor’s PPE.
Cost vs Effectiveness & Experience
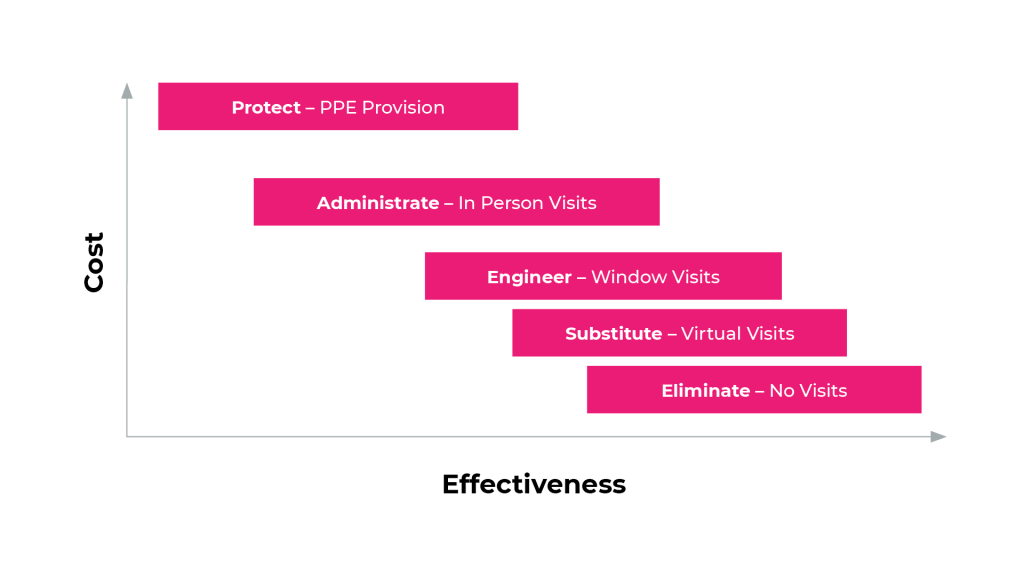
As you can see in the chart above, cost increases as effectiveness drops.
So, Eliminate will be more effective and less costly than Engineer. Engineer will be likewise more effective and less costly than Protect.
However, more effective methods can disrupt customer experience.
For example, it would be simplest and most cost effective to cut resident visits altogether, but as we’ve shown, this isn’t sustainable.

The Hierarchy of Control shows here that an aged care home can substitute physical visits for less risky virtual visits and window visits, while still maintaining a good customer experience.
Conclusion
COVID-19 has scarred but refined aged care. Australian aged care facilities now have:
- robust infection control procedures
- increased infection control training, and
- better risk management practices.
As aged care progresses, more and greater innovations will be made in infection control. Australian aged care homes can and will protect their residents, even while maintaining great customer experience.
The Hierarchy of Control, based on proven WHS principles, is invaluable for risk management and innovation.